![DRAFT Clinical Evidence Supporting DermaSensor AI Skin Cancer Risk Detection – [Duplicated]](https://www.dermasensor.com/wp-content/uploads/iStock-1618263235-2048x2048.jpg)
Clinical Evidence Supporting DermaSensor’s AI Skin Cancer Risk Detection
Clinical decision-making requires certainty, yet the visual assessment of skin lesions often leaves room for doubt. For physicians, the challenge is balancing the need to catch malignancies early while also trying to avoid unnecessary, invasive procedures.
For clinicians evaluating a new diagnostic tool, the evidence has to be clear. DermaSensor is supported by multiple prospective, multi-center studies demonstrating melanoma detection accuracy and performance across all three common skin cancers.
This page summarizes the key clinical data, including pivotal trial results, FDA clearance, and real-world primary care evidence, to support your evaluation
Quick Facts About Clinical Evidence Supporting DermaSensor
96% Sensitivity
Demonstrated sensitivity for detecting all common skin cancers in pivotal clinical trials.
FDA-Cleared
The first automated, point-of-care device indicated for BCC, SCC, and melanoma.
High NPV
Features a 98% negative predictive value (NPV) for melanoma, providing high confidence when a "Monitor" result is issued.
Validated on 20,000+ Scans
Algorithm developed and validated through clinical studies on thousands of biopsy-proven lesions.
What is the clinical evidence for DermaSensor's accuracy?
The clinical evidence for DermaSensor is anchored by multiple prospective, multi-center studies demonstrating a 96% sensitivity for detecting all skin cancers. This performance was validated against the gold standard of dermatopathology across more than 1,000 patients in pivotal trials. The data confirms that the device provides highly reliable, objective information to help clinicians determine whether suspicious skin lesions require further clinical care.
Closing the Diagnostic Gap
Visual inspection alone is subjective. For many providers, this uncertainty leads to “defensive medicine,” where benign lesions are referred or biopsied “just in case.” One in five Americans will develop skin cancer by age 70*, making early and accurate triage a critical priority for patient outcomes. DermaSensor provides an objective spectral result that reduces the uncertainty at the point of care.
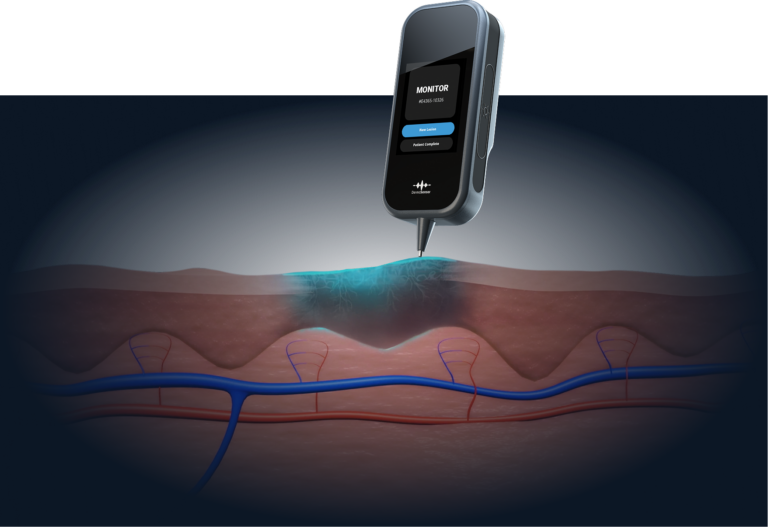
How the Technology Works
Unlike image-based tools, DermaSensor uses Elastic Scattering Spectroscopy (ESS). This technology analyzes the cellular and sub-cellular structure of a lesion by measuring how light bounces off the tissue. This approach evaluates physical properties invisible to the human eye, providing AI skin cancer detection accuracy that goes beyond surface-level visual assessment.
Learn More about
Melanoma Detection Accuracy and Pivotal Trial Results
Because melanoma is the deadliest form of skin cancer, melanoma detection accuracy remains the most critical metric for any new clinical tool. DermaSensor's performance data comes from rigorous, multi-center prospective studies.
DERM-SUCCESS: Primary Care Study
In the DERM-SUCCESS study, the device was evaluated on over 10,000 lesion assessments and 108 U.S. Board Certified PCPs. Device use resulted in a significant improvement in both management and diagnostic sensitivity compared to standard of care alone; physician false negative referrals decreased by half, from 18.0% to 8.6%.
- PCPs' device-assisted accuracy (i.e. AUROC) was 76%, compared to 71% with their standard of care alone.
- For lesions in which PCPs had low confidence in their clinical management decision, their device-assisted accuracy was 68% and unassisted was 57%.
Nearly all (99%) of PCP participants reported the device provides at least one benefit, including:
- "Detecting more skin cancer" (82%)
- "Providing you with greater confidence in your clinical assessments and management decisions" (81%)
- "Helping you to prioritize the risk level of concerning lesions to prioritize patient management, e.g. a prioritized dermatology referral" (72%)
- "Increasing your frequency of assessing patients for skin cancer" (63%)
DERM-ASSESS III: Dermatology Study
The DERM-ASSESS III melanoma clinical utility study, published in JCAD, consisted of 118 PCPs who completed assessments of over 10,000 lesion cases.
- Physician AUC improved significantly with the use of DermaSensor, from 0.630 to 0.671 (p = 0.036) [1].
- Melanoma detection increased from 70.2% to 79.1%, decreasing missed melanoma from 29.8% to 20.9% [1,2].
Reference:
1. Seiverling, E.V. (2025). JCAD MRMC Study. Journal of Clinical and Aesthetic Dermatology, October 2025, 58-65. Link
2. DermaSensor Inc. (2025). FDA Clearance and AI-Powered Device Overview.
Performance in Primary Care
The DermaSensor clinical evidence highlights a significant improvement in the primary care workflow, Their relative decrease in false negative referrals (i.e., missed skin cancers) decreased by 30-52%. This evidence supports the device as a vital safety net for those on the front lines of patient care.

AI Skin Cancer Detection Accuracy Across Various Clinical Settings
A clinical tool must perform consistently across different patient populations and clinician experience levels to be truly effective. DermaSensor has been evaluated in both primary care and dermatology settings.
Dermatologist-Level Sensitivity
In a prospective dermatology study, the device was shown to maintain sensitivity comparable to dermatologists (95.5% device vs 90% dermatologist sensitivity). For a non-specialist, this means having access to an expert-level "second look" during a standard skin check.
To learn more about this study click here
Reliability Across Cancer Types
The AI melanoma detection accuracy is matched by its performance in detecting non-melanoma skin cancers. In independent studies, the device identified 100% of malignant lesions evaluated, including:
- Melanomas
- Basal Cell Carcinomas (BCC)
- Squamous Cell Carcinomas (SCC)
This consistency ensures that the device is a comprehensive tool for evaluating skin lesions suggestive of malignancy.
Interpreting the AI Results
DermaSensor does not provide a diagnosis; it provides an objective assessment of risk to support your clinical judgment.
The Scoring System
For results labeled "Investigate," the device provides a score from 1 to 10.
Low Scores (1-5)
Suggest lower spectral similarity to malignant lesions.
High Scores (7-10)
Lesions with high spectral similarity (scores 7-10) were markedly more likely to be malignant.
This scoring system provides clinicians with a clear, quantifiable framework for making referral or biopsy decisions. By providing this level of AI skin cancer accuracy, the device helps reduce the friction often found in the triage process.
Integrating Evidence into Clinical Practice
DermaSensor is built to meet the evidence standards clinicians require before adopting a new diagnostic tool.
FDA Clearance
DermaSensor is the first FDA cleared automated device for all three common skin cancers.
Workflow Efficiency
The device delivers automated results in seconds, fitting into the typical primary care or specialty visit without disrupting patient flow.
Reimbursement Support
We provide dedicated support to help you document these evidence-based assessments.
Ready to review the full clinical data behind DermaSensor for your practice?
Or
To request a full compendium of our published clinical studies and whitepapers
Skin Cancer Detection Accuracy - FAQs
DermaSensor Clinical Evidence: Frequently Asked Questions
What is the proven skin cancer risk detection accuracy of DermaSensor?
DermaSensor demonstrated 96% sensitivity for detecting all common skin cancers in its pivotal clinical trials. This high skin cancer detection accuracy helps ensure that malignant lesions are correctly flagged for further clinical investigation.
What clinical studies support DermaSensor’s performance?
DermaSensor’s performance is supported by multiple prospective, multi-center studies, including the DERM-SUCCESS pivotal trial across 22 study centers. These studies demonstrated 96% sensitivity for detecting all common skin cancers, validated against gold-standard dermatopathology.
How does DermaSensor support melanoma detection accuracy?
The device has a 98% negative predictive value (NPV) for melanoma, providing high confidence when a “Monitor” result is issued. It is the first FDA-cleared automated device indicated for melanoma, BCC, and SCC.
What does the DermaSensor clinical evidence say about missed cancers?
In clinical studies, when PCPs used the device, their relative decrease in missed skin cancers (false negative referrals) was between 30% and 52%. This significantly improves the safety and reliability of the primary care skin check.
Is the AI skin cancer detection accuracy of DermaSensor consistent across different cancer types?
Yes, the device is the first FDA-cleared automated tool indicated for Melanoma, Basal Cell Carcinoma, and Squamous Cell Carcinoma. In various studies, it has shown reliable sensitivity across all three categories.
How was the AI algorithm developed and validated for DermaSensor?
The DermaSensor device result is determined using a proprietary machine-learning algorithm that has been developed and validated through clinical studies on thousands of diagnosed lesions. It was trained on a database of over 20,000 scans to ensure robust performance.
Does the DermaSensor device replace the need for a biopsy?
No, the DermaSensor device is intended to assist the user in deciding whether skin lesions require further clinical care and is not intended to be used for the direct diagnosis of skin cancer. It provides objective information to inform your clinical decision-making.
Is there a study comparing DermaSensor to dermatologist performance?
Yes, in a prospective study, the device maintained sensitivity comparable to dermatologists, showing 95.5% device sensitivity vs 90.9% dermatologist sensitivity. This makes it an ideal tool for clinicians looking for objective diagnostic support.
How does DermaSensor’s sensitivity compare across care settings?
DermaSensor has been evaluated in both primary care and dermatology settings. In primary care studies, PCPs’ sensitivity to skin cancer increased by 6-9% when using the device alongside their clinical assessment.
Confidence Backed by Clinical Evidence
Request a demo to see how DermaSensor’s clinical performance translates to your patient evaluations.